In General How Does High Blood Pressure Damage The Heart?
The heart pumps blood to the entire body. Uncontrolled high blood pressure can damage the heart in a number of ways, such as:
- Coronary artery disease
Coronary artery disease affects the arteries that supply blood to the heart muscle. Arteries narrowed by coronary artery disease don’t allow blood to flow freely through the arteries. When blood can’t flow freely to the heart- chest pain, a heart attack or irregular heart rhythms (arrhythmias) can occur.
- Enlarged left heart
High blood pressure forces the heart to work harder than usual in order to pump blood to the rest of the body. This causes the left ventricle to thicken or stiffen (left ventricular hypertrophy). These changes limit the ventricle’s ability to pump blood adequately. This condition increases your risk of heart attack, heart failure and sudden cardiac death.
- Heart failure
Over time, the strain on the heart caused by high blood pressure can cause the heart muscle to weaken and work less efficiently. Eventually, the heart simply begins to wear out and fail. Damage from heart attacks adds to this problem.
What Is The Relationship Between High Blood Pressure And Coronary Artery Disease?
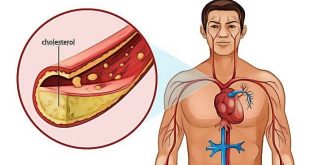
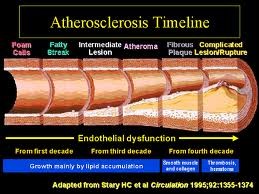
One of the most serious health problems related to untreated high blood pressure is atherosclerosis, or plaque build-up in the arteries. When those blockages occur in the arteries that supply blood to the heart muscle, the end result is called coronary artery disease.
When the heart beats, it pushes blood through the arteries in the entire body. Higher blood pressures mean that with each beat, arteries throughout the body swell and stretch more than they would normally. This stretching can injure the endothelium, the delicate lining of all arteries, causing arteries to become stiffer over time.
Healthy endothelium actively works to prevent atherosclerosis – also called hardening of the arteries – from developing. Injured endothelium, on the other hand, attracts more “bad” LDL cholesterol and white blood cells. The cholesterol and cells build up in the artery wall, eventually forming the plaque of atherosclerosis.
The narrowed artery limits or blocks the flow of blood to the heart muscle, depriving the heart of oxygen.
Plaque is dangerous. It often grows without symptoms for years. When the process is advanced enough, patients can experience angina, or chest pain, when they exert themselves. The hardened surface of the artery can also encourage the formation of small blood clots, potentially leading to a heart attack or stroke.
What Are the Symptoms Of Coronary Artery Disease?
Atherosclerosis usually has no symptoms until the narrowed coronary arteries severely restrict blood flow to the heart. At this point, there may be chest pain -because not enough blood is reaching the heart, especially while you are exerting yourself or are under stress.
How Is Coronary Artery Disease Diagnosed?
Coronary artery disease isn’t usually diagnosed until a person complains of chest pain. At this point, the doctor may conduct tests to evaluate your risk for heart disease. These tests include:
- Electrocardiogram (EKG or ECG): This test measures the electrical activity, rate, and rhythm of your heartbeat via electrodes attached to your arms, legs, and chest. This test may show if you’ve had a heart attack in the past or if you are currently having a heart attack, strain, or thickening of the heart muscle.
- Exercise stress test: During this test, you exercise on a stationary bicycle or treadmill to increase your heart rate and blood pressure while EKG readings are taken. This test is often performed with imaging techniques, such as an echocardiogram or nuclear scans, to provide better detection of heart disease.
- Cardiac catheterization: During this procedure, a catheter — a small flexible tube — is inserted into an artery and guided up to the coronary arteries, at which point dye is injected through the tube and observed as it flows inside those arteries. This allows the doctor an opportunity to directly locate and measure any blockages in the coronary arteries. During a cardiac catheterization, a cardiologist may also be able to open up any clogged arteries detected with a procedure called an angioplasty. This may also involve expanding a small metal mesh tube, called a stent, inside the blood vessel to better prop the artery open.
- Echocardiogram: This test uses ultrasound waves to provide pictures of the heart’s valves and chambers, giving information about chamber size and wall thickness and how blood is flowing within the chambers. Because this is such a safe, comprehensive and readily available evaluation, the echocardiogram is often used as the first test (after an EKG) to look for evidence of underlying heart problems. The coronary arteries are not seen during an echocardiogram, so unless a heart attack has already affected the heart, the presence of blockages cannot be made or excluded based upon this test alone.
- Computed tomography (CT) scan: An X-ray and a computer are used to construct a cross-sectional image of the heart. This can provide information about the presence of calcium in heart arteries (an indication of underlying atherosclerosis). Some CT scanners are also able to provide much more detailed pictures of the heart arteries, yielding information similar to that obtained from a coronary angiogram.
- Cardiac Magnetic resonance arteriography (CMRI): This test provides images scarring in the walls of the heart which might indicate coronary artery disease.
Treatment
- Lifestyle changes (such as a healthy diet and regular physical activity) are essential for preventing and treating CAD.
- Treating risk factors like hypertension, diabetis can reduce the chances of getting heart attack and stroke.
- Medications for preventing and treating CAD include aspirin, cholesterol-lowering drugs (statins), and high blood pressure medications. Some patients take nitrate drugs such as nitroglycerin or other medications to treat angina.
- Procedures may be needed to open blocked or narrowed coronary artery and improve blood flow to the heart. This approach is known as reperfusion therapy. Percutaneous coronary intervention (PCI), also called angioplasty, uses a small balloon to open the blood vessel. Coronary artery bypass graft (CABG) is a more invasive procedure that is generally recommended for patients with severe heart disease. It uses grafts from arteries or veins to reroute blood flow.
References
- http://www.mayoclinic.org/disease
- Coronary artery disease | University of Maryland Medical Center http://umm.edu/health/medical/reports/articles/coronary-artery-disease#ixzz3Bfe2IZTg
University of Maryland Medical Center Follow us: @UMMC on Twitter | MedCenter on Facebook
| Last Reviewed | : | 18 September 2017 |
| Writer | : | Dr. Ainol Shareha Binti Sahar |
| Translator | : | Dr. Ainol Shareha Binti Sahar |
| Accreditor | : | Dr. Zarina Banu Binti Abdulla |
 PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia
PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia