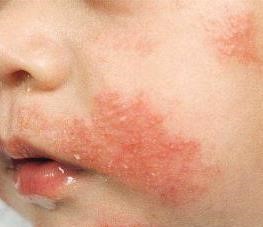
Asthma and Eczema
Childhood eczema (allergic dermatitis) is associated with other allergic diseases such as hay fever, food allergies, and asthma. Eczema may be the first sign of allergies in a child. Half of children with asthma also have eczema. Eczema does not cause asthma or other allergic diseases..
How Can It Be Treated?
While there is no cure for eczema, you can take steps to manage your symptoms and lessen the severity of outbreaks.
- Treatment begins with efforts to reduce the itching and inflammation, hydrating the skin and removing the “flare factors” such as infections and exposure to allergens and irritants:
- Bath in warm water not hot water for no more than 3-5 minutes. Use unscented soap or soap substitute. Pat the skin dry, then promptly apply a moisturizer. This will help keep the skin hydrated. If the area has become thick, moisturizing ointments are used.
- Trim fingernails to reduce problems from scratching. At night, patients can wear cotton socks on their feet or gloves on their hands to prevent scratching while asleep.
- If the rash is oozing, doctors may prescribe a lotion to dry the rash and an antibiotic to treat infection. If the rash is on the face, do not use a corticosteroid product.
- Stay indoors, in air conditioning on hot weather. This avoids sweating and the itchiness it causes.
- Avoiding activities that make you hot and sweaty as well as abrupt changes in temperature and humidity.
- Maintaining cool temperatures in sleeping areas, because heat can lead to sweating that worsens itching and irritation.
- Avoid wool, polyester, wrinkle-resistant, flame-retardant or scratchy fabrics in clothes and bedding. Wear open-weave, loose fitting cotton or cotton blend garments. Wash new clothes before wearing.
- Reduce indoor allergens, particularly dust mites, by washing bedding in hot water, removing rugs, stuffed furniture, stuffed toys and curtains where possible.
- When doing housework, wear plastic or rubber gloves or latex gloves lined with cotton.
- Avoid stress, which can add to flare-ups.
- If a link with food has been diagnosed, eliminate it from the patient’s diet. This will reduce symptoms, but not always get rid of them.
- Use liquid laundry detergent that is unscented and mild.
Avoid fabric softeners (liquid and dryer sheets). Rinse clothing and bedding thoroughly after washing to remove detergent residue.
- Avoid chemicals and extreme heat or cold, which can worsen the condition.
- Practicing good skin hygiene even when you are not having symptoms.
- Patients often feel angry and frustrated by the chronic itching. Parents need to find ways to let children with atopic dermatitis express feelings. With proper treatment the condition can be controlled and most of the time it will improve with age. There are many methods available to reduce stress.
What About Medication?
- Topical steroids are key medications for controlling the itching and inflammation. Used immediately after bathing, they also help keep the skin hydrated. Most steroids require a prescription. Systemic corticosteroids (tablets, shots or liquids) should seldom be used. They cause flare-ups when the medications are discontinued.
- Anti-histamines may help relieve itching, often sedating the patient. They are most useful when given at bedtime.
- Antibiotics will treat complicating skin infections. Impetigo is usually treated with oral antibiotics or, if the case is mild, topical antibiotics. Healing should begin in three days.
 PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia
PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia