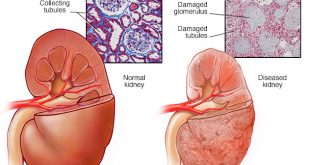
Introduction
The prevalence of Chronic Kidney Disease (CKD) & End-Stage Kidney Disease (ESKD) is increasing worldwide. In Malaysia, the incidence & the prevalence of patients on dialysis has increased to 234 & 1155 pmp respectively in 2014 as compared with 88 & 325 pmp respectively in 2001. 1
CKD is an enormous human, economic and social burden on the healthcare system. The most important step is early detection and intervention to prevent progression to ESKD.
Strategies to retard the progression of CKD
- Optimal blood pressure control
- Target blood pressure (BP) should be <130/90
- Aim for Systolic BP range 120 – 129 mmHg
- Angiotensin-Converting Enzyme Inhibitor (ACEi)/Angiotensin Receptor Blocker (ARB) should be used as the first-line agent if there is proteinuria (loss of protein in urine)
- May require multiple drugs to achieve target blood pressure
- Treatment of ‘microalbuminuria/proteinuria’
- Retardation of progression of kidney failure correlates with the degree of proteinuria reduction
- Reduction of ‘proteinuria’ to at least 60 percent of baseline values should be targeted to be effective
- Angiotensin-Converting Enzyme Inhibitor (ACEi)/Angiotensin Receptor Blocker (ARB) should be used as the first-line agent
- Non-dihydropyridine Calcium channel blocker (CCB) anti-hypertensive agents have a greater antiproteinuric effect than dihydropyridine (DHP) CCB.
- Non-dihydropyridine CCBs can be alternative for those that are intolerant/contraindicated to ACEi or ARB or in combination within ACEi or ARB for additional proteinuria reduction is required.
Other targets:
- Glycemic control
- Diabetic Kidney Disease accounts for 58% of new patients starting dialysis
- The target HbA1c should be ? 7% in patients with diabetes but individualised according to presence of other diseases in the same patients
- Lowering HbA1c to approximately 6.5% to 7% reduces the development of ‘microalbuminuria’ and overt ‘proteinuria’
- In the presence of chronic kidney disease, the dose of hypoglycemic agents should be adjusted to avoid low blood sugar level.
- Correction of abnormal lipid levels
- Full lipid profile should be performed at least annually
- More frequent monitoring is indicated after commencement of treatment to achieve target levels
- Therapeutic lifestyle changes should be instituted if LDL cholesterol is more than 2.6 mmol/l
- Drug therapy should be considered if LDL-cholesterol is more than 3.4 mmol/l
- Target to achieve: LDL cholesterol is less than 2.6 mmol/l
- Statin should be offered to patients with chronic kidney disease for primary and secondary prevention of cardiovascular events
- Antiplatelet agent
- CKD is a recognised risk factor for the development of CVD
- Patient with CKD is often prescribed antiplatelet medications
- Aspirin should be used in patients with DN for secondary prevention of cardiovascular disease
- Combination of clopidogrel with aspirin should be avoided in patients with diabetic nephropathy
Summary
There is no single treatment in the prevention of CKD. We need to control many targets (blood pressure/ proteinuria/ HbA1c/ lipid level) in retarding progression of CKD.
References
- Lim YN et al. 22nd Report of the Malaysian Dialysis and Transplant Registry 2014. Kuala Lumpur, National Renal Registry. 2011
- Malaysian Clinical Practice Guideline: Diabetic Nephropathy July 2004
- Malaysian Clinical Practice Guideline: Management of Chronic Kidney Disease in Adult 2011
| Last Reviewed | : | 24 June 2016 |
| Writer | : | Dr. Shahnaz Shah Firdaus Khan |
| Accreditor | : | Dr. Wong Hin Seng |
 PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia
PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia