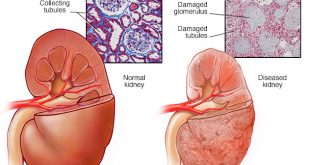
What is kidney transplant rejection?
It is the most common complication after the kidney transplantation. Our body immunity is to fight any invader into the body. When an organ like a kidney is transplanted into a patient (recipient), the recipient’s immune system will detect the new kidney ( graft ) as being foreign, and try to fight against it. The recipient’s immune system will damage the transplanted kidney leading to impaired graft function and possible failure of the transplanted organ.
Who will get rejection in kidney transplant?
Rejection has the potential to occur in every kidney transplant recipient.
How common does rejection occur?
In the era of 1980s when we did not have potent immunosuppressant medications, acute rejection episode occurred in almost 50-60% of kidney transplants . However, with improved medications available, the incidence of acute rejection is now about 10% (United States Renal Data System , 2009).
The majority of the acute rejection episodes occur in the first 6 months after the transplant but even many years after the transplant there is a possibility of acute rejection occurring, particularly in patients who are non-adherent to the immunosuppressive medications prescribed.
How do episodes of rejection occur?
The rejection episodes occur as a result of the immune reactions of the recipient. These episodes can happen due to acute or chronic processes involving cells from the immune system adhering to the graft and causing damage to it.
How we reduce the risk of rejection?
The rejection risk can be reduced by:
- Better matching the donor and recipient blood group and tissue type, for example, a donated organ from siblings, parents and close relatives would usually be well-matched with the recipient compared to an organ from someone unrelated.
- Donor and recipient having compatible blood groups .
- Use of immunosuppressant medication.
- Regular monitoring of kidney function and adherence to the medication.
What are the symptoms of rejection?
Rejection can occur without symptoms and this is why regular monitoring by your doctor is important. In cases of severe acute rejection, however, you may notice reduced urine output, discomfort at the site of the organ, fever, and urine abnormality.
There are 3 types of rejection:
- Hyperacute rejection occurs within a few minutes to hours after the transplant. This type of rejection is rare but can occur if the recipient has preformed antibodies against the transplanted organ. These preformed antibodies may be induced by prior blood transfusions, multiple pregnancies or prior transplantation.
- Acute rejection may occur any time most commonly in the first 6 months after transplant.
- Chronic rejection is a gradual process occuring over months to years. The recipient’s immune system slowly damages the transplanted organ.
Your doctor will perform a cross-match test between the donor and recipient before transplant to detect if there is any risk of this occurring.
How can we diagnose rejection?
The possibility of a rejection episode occurring can be detected early by regular blood investigations. To confirm the diagnosis, your doctor will need to do a graft biopsy and examine the biopsy specimen by microscopy with special staining. Your doctor will then be able to classify the type of rejection according to the findings and manage the rejection episode appropriately .
Because rejection episodes commonly occur in the first 6 months after transplant, the patient will need frequent blood and urine monitoring during this early period after transplant.
Is there treatment available for rejection?
Yes. The doctor will treat the rejection according to biopsy finding and severity. The purpose of the treatment is to suppress the immune system.
What are the types of treatment available?
High doses of steroid are usually given initially . If the high dose steroid fails, your doctor will need to use moe powerful anti-rejection medications such as anti-thymocyte globulin (ATG) .
Your doctor will also intensity use of immunosuppressants, for example, keep blood levels of agents from the CNI group higher, or change to a more powerful medication.
If the rejection is due to recipient antibody production, your doctor will need to perform plasmapheresis which is a process to remove the recipient antibodies that are attacking the organ.
What will happen after an episode of organ rejection?
The organ function might be reduced temporarily. Successful treatment will restore function, although sometimes the recovery of function may not be full.
What other possible complications can occur after organ rejection?
In the worst case scenario, there may be a complete loss of function in the transplanted organ and it may become necessary to commence on dialysis. The recipient will also be at risk of side effects of the increased levels of immunosuppressive medications which include increased susceptibility to severe infection and long-term risk of malignancy.
Is it possible to get another rejection after treatment of rejection?
Yes. If a recipient is non-adherent to immunosuppressive medications or undertreated, recurrent rejection can occur. Your doctor will need to balance between the side effect of medication and rejection risk.
Can a recipient get another transplant if the previous graft fails due to rejection?
Yes. The patient can have another transplant as long as there is no contraindication.
Does the failed transplanted kidney need to be removed?
Your doctor will need to discuss with you in detail regarding the risk of surgery to remove a failed graft as against the risk of retaining the graft .
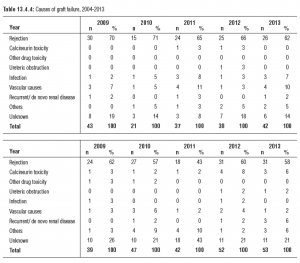
Reference
- 21st Report of the Malaysian Dialysis and Transplant Registry 2013. Retrieved from: http://www.msn.org.my/Doc/PublicDoc_PB/Publication/mdtr2013/Chapter02_(erratum).pdf
| Last Reviewed | : | 27 July 2016 |
| Writer | : | Dr. Yaw Chong Hwa |
| Accreditor | : | Dr. Liu Wen Jiun |
 PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia
PENDIDIKAN PESAKIT Kementerian Kesihatan Malaysia